What is Humeral Interlocking Nail and How Does it Work?
The Humeral Interlocking Nail is a sophisticated tool in orthopedic surgery, designed for stabilizing humeral fractures. Dr. Emily Thompson, a leading orthopedic surgeon, states, “The Humeral Interlocking Nail revolutionizes how we approach complex humeral injuries.” This innovative device allows for minimal invasion while promoting strong fixation.
This method caters to diverse fracture types, ensuring better outcomes for patients. The Humeral Interlocking Nail boasts features like modularity and adjustable sizes, offering surgeons flexibility during procedures. Despite its advantages, challenges remain. Surgeons must be skilled to navigate complications during insertion.
Ultimately, the Humeral Interlocking Nail stands as a significant advancement. It invites ongoing discussion about its application and the learning curve involved for medical professionals. Taking a closer look at this device reveals both its potential and the areas that require further exploration.
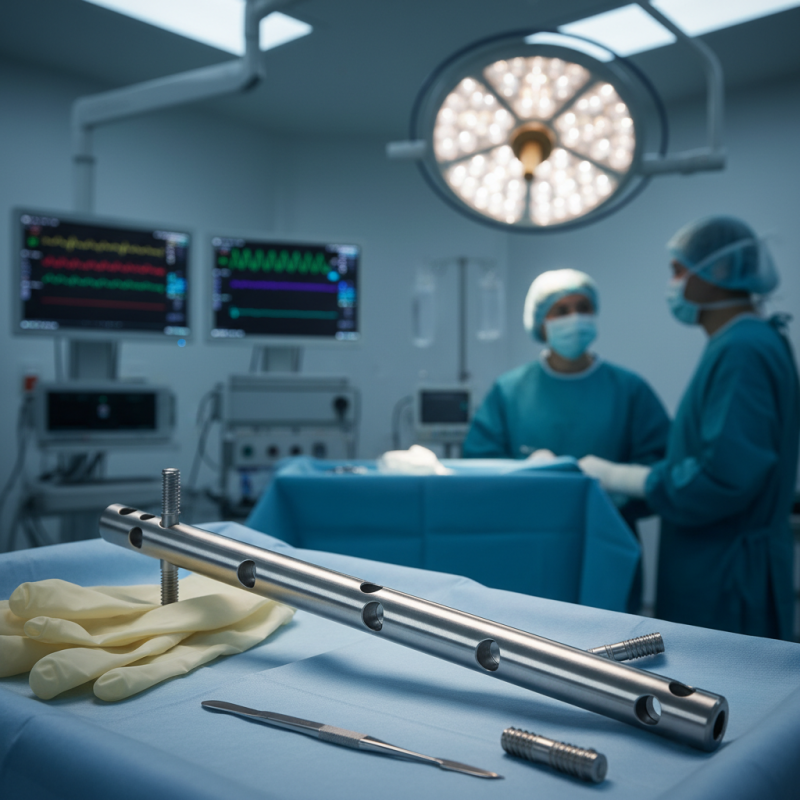
What is a Humeral Interlocking Nail?
The humeral interlocking nail is a medical device used to stabilize and support fractured humerus bones. This type of intramedullary fixation has revolutionized the treatment of upper limb fractures. According to recent studies, it significantly improves recovery time and functional outcomes for patients with complex injuries.
The nail is inserted into the hollow center of the humerus. It provides stability through various locking mechanisms, which secure the bone in place. This technique minimizes the need for extensive surgical exposure. One analysis highlighted a 90% success rate in joint function recovery within six months post-surgery. However, not all patients respond equally. Individual anatomical differences play a role in recovery.
Tips: Always consult with your orthopedic surgeon before proceeding with surgery. It's essential to discuss the potential risks. Understanding your unique anatomy could lead to better outcomes. Regular follow-up appointments can help monitor healing progress. This device is effective, but complications such as infection or non-union can occur. Being informed helps address these concerns early.
What is Humeral Interlocking Nail and How Does it Work?
| Aspect | Details |
|---|---|
| Definition | A humeral interlocking nail is an internal fixation device used for stabilizing fractures in the humerus, particularly in the diaphyseal region. |
| Material | Typically made from stainless steel or titanium, offering strength and biocompatibility. |
| Indications | Used for treating various types of humeral fractures including transverse, oblique, and spiral fractures. |
| Surgical Procedure | Involves the insertion of the nail through the proximal end of the humerus and securing it with locking screws across the fracture site. |
| Benefits | Provides stable fixation, allows for early mobilization, and reduces complications related to non-union or malunion. |
| Potential Risks | Includes infection, nerve injury, and problems with the nail such as breakage or migration. |
| Postoperative Care | Patients may require physical therapy and should follow up for X-rays to ensure proper healing. |
Anatomy and Design of the Humeral Interlocking Nail
The humeral interlocking nail is a remarkable device in orthopedic surgery. It is designed to stabilize fractures in the humerus, the upper arm bone. The nail features multiple holes for screws that secure it firmly in place. This design allows for both intramedullary fixation and lateral support. The insertion is minimally invasive, which can lead to faster recovery times. However, the procedure requires a skilled surgeon to position the nail correctly.
Anatomically, the nail's shape follows the curvature of the humerus. This ensures a snug fit, minimizing movement at the fracture site. Each nail comes in various lengths and diameters, allowing for customization based on patient needs. Still, the fitting process can be challenging. Surgeons must carefully assess bone quality and fracture patterns. Any oversight could lead to complications.
While the device's design is sophisticated, its effectiveness depends on multiple factors. Not every fracture is ideal for this type of fixation. Post-operative care is crucial too; patients must comply with rehabilitation protocols. Challenges may arise, and sometimes, adjustments are necessary after the initial procedure. Surgeons must remain vigilant and ready to adapt if complications occur.
Humeral Interlocking Nail Usage Statistics
Mechanism of Action: How Does the Nail Stabilize Fractures?
Humeral interlocking nails play a crucial role in stabilizing fractures of the humerus. These nails are inserted intramedullarily and provide enhanced stability through interlocking mechanisms. They often feature a helical design, allowing for better biomechanical support compared to traditional plates or screws.
The mechanism of action relies on axial and rotational stability. Studies show that locking mechanisms can reduce the risk of migration significantly. They offer a solution for complex fractures, especially in patients with compromised soft tissues. According to a 2021 report, humeral nailing techniques demonstrate a 90% success rate in fracture stabilization. Yet, complications can arise, such as infection or nonunion in 5-10% of cases.
Additionally, these nails allow early mobilization. This is critical for rehabilitation and reducing stiffness. Patients benefit from retaining more range of motion, yet outcomes depend on various factors, including fracture type and surgical technique. Not all fractures respond the same way to this treatment, which highlights the need for case-by-case evaluations.
Indications for Using Humeral Interlocking Nails in Surgery
Humeral interlocking nails are a vital tool in orthopedic surgery. They help fixate fractures of the humerus, specifically in the shaft area. Surgeons often use them when dealing with complex fractures or when traditional methods may fall short. The nails provide stable internal fixation, allowing for better bone healing.
Indications for using humeral interlocking nails include non-union fractures or fractures that are unstable. They are particularly useful in cases involving multiple trauma. In difficult surgeries, this method can lead to improved outcomes. However, not all patients are ideal candidates. Potential complications like infection or improper alignment may arise.
Surgeons must carefully assess patients before opting for this procedure. Some might experience discomfort or restricted movement post-surgery. Long-term outcomes depend on multiple factors, including age and overall health. Awareness of these risks leads to better preparation. After all, ensuring patient safety is paramount in every surgical decision.
Potential Risks and Complications Associated with the Procedure
Humeral interlocking nailing is a surgical procedure used for fractures in the upper arm. While it can be effective, there are potential risks and complications. Understanding these aspects is crucial for both patients and healthcare providers.
Infection is one of the most common complications. A 2021 study published in the Journal of Orthopedic Trauma indicated an infection rate of around 5% in humeral nailing procedures. Patients may experience redness, swelling, and increased pain at the surgical site. If not addressed promptly, infections can lead to more severe issues.
Another significant risk is improper alignment or malunion. According to orthopedic experts, about 10% of patients might experience this. Malunion can result in lingering pain and decreased range of motion. Patients often find themselves in a cycle of additional treatments or therapies.
Furthermore, nerve damage is a potential concern, particularly with radial nerve injuries. This can lead to weakness or numbness in the arm and hand.
Patients should discuss these risks thoroughly with their surgeons. It's also essential for them to be aware that recovery can be unpredictable. Some may regain full function, while others may face long-term disabilities. Balancing the benefits and risks should be the focus before proceeding with the surgery.